
COMMON EYE PROBLEMS
Disclaimer: The information provided is for patients and their families to learn general information about common eye conditions. Your eye care professional who has examined the patient’s eyes and is familiar with his or her medical history is the best person to answer specific questions.

Cataracts

A cataract is a clouding of the lens in the eye. Most cataracts are related to aging and are very common in older people. By age 80, more than half of all Americans either have a cataract or have had cataract surgery. A cataract can occur in either or both eyes. It cannot spread from one eye to the other. A cataract can affect vision in several ways.
The most common symptoms of a cataract are:
-
Cloudy or blurry vision.
-
Colors seem faded.
-
Glare (headlights, lamps, or sunlight may appear too bright
-
Halos around lights.
-
Poor night vision.
-
Double vision or multiple images in one eye. (This symptom may clear as the cataract gets larger.)
-
Frequent prescription changes in your eyeglasses or contact lenses.
These symptoms also can be a sign of other eye problems. If you have any of these symptoms, check with your eye care professional.
The symptoms of early cataract may be improved with new eyeglasses, brighter lighting, anti-glare sunglasses, or magnifying lenses. If these measures do not help, surgery is the only effective treatment. Surgery involves removing the cloudy lens and replacing it with an artificial lens.
You and your eye care professional can make the decision together about when is the right time to have cataract surgery. One aspect of the decision to remove a cataract is how much the decrease in vision and visual quality interferes with your everyday activities, such as driving, reading, or watching TV. Once you understand the benefits and risks of surgery, you can make an informed decision about whether cataract surgery is right for you. Sometimes a cataract should be removed even if it does not cause problems with your vision. For example, a cataract should be removed if it prevents examination or treatment of another eye problem, such as age-related macular degeneration or diabetic retinopathy. In most cases (but not all), delaying cataract surgery will not cause long-term damage to your eye or make the surgery more difficult, and you do not have to rush into surgery.
Once you and your doctor decide to schedule cataract surgery, our office will help you coordinate a physical exam with your primary care doctor to clear you for anesthesia and surgery. We will also arrange an appointment at our office for preoperative measurements and paperwork, and write you a prescription for eye drops to use before and after the surgery. Your surgery will take place either at Fairbanks Memorial Hospital or the Surgery Center of Fairbanks. If you have cataracts in both eyes that require surgery, the surgery on each eye will be performed on separate days. Generally you will have a postop appointment at our office the next day and in 1 week after surgery to check your vision and monitor the healing progress. Most patients are able to get a new eyeglasses prescription about 4-6 weeks after having cataract surgery.
Diabetic Eye Disease

Diabetic retinopathy is a leading cause of blindness in American adults. It is caused by damage to the blood vessels of the retina as a result of high blood sugars. In some people with diabetic retinopathy, retinal blood vessels may swell and leak fluid, in others the blood vessels can become blocked and no longer let blood through. Still In other people, abnormal new blood vessels grow on the surface of the retina. These new blood vessels can bleed into the eye, or can cause traction on the retina and lead to a retinal detachment. In addition, patients with diabetes are more likely to form a cataract at a younger age than their peers without diabetes, and the cataract is often of the kind that grows relatively quickly and causes significant visual decline. Any of these changes may result in decreased vision and can even lead to blindness.
Diabetic eye disease often has no warning signs that a patient would notice until late in the disease. Blurred vision may occur when the macula (the part of the retina that provides sharp, central vision) swells from the leaking fluid. This condition is called macular edema. If new vessels have grown on the surface of the retina, they can bleed into the eye (vitreous hemorrhage), causing a loss of vision. In patients with severe disease or in those whose vision is affected by diabetic retinopathy, there are treatments that can be applied, such as laser, an injection into the eye, or even surgery.
While laser surgery, injections, surgery, and appropriate follow-up care can reduce the risk of blindness by 90 percent, none of the treatments applied can “cure” the retinopathy. The source of the damage in the retina in high blood sugars, which need to be controlled to have any chance of limiting further progression of the disease. As there is no pain with diabetic retinopathy and vision may not change until the disease becomes severe, if you have diabetes it is important that you get a dilated eye examination at least once a year. Finding the disease early will allow for appropriate follow-up and treatment to help limit the damage to the retina from diabetes. Knowing the status of your disease is also important as you and your primary care doctor seek to make improvements to your blood sugar control regimen, including healthy eating choices, exercise and medications, to prevent worsening of the disease.
Macular Degeneration
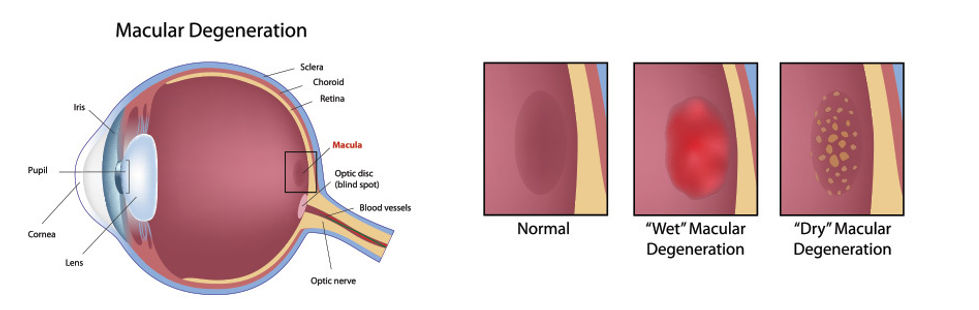
Macular Degeneration, also called age-related macular degeneration (AMD), is a leading cause of vision loss in Americans age 60 years and older. Our retina is the layer of tissue that lines the inside of the eye and receives the light/images that come into the eye and transfers the images via the optic nerve to the brain. The macula is the area or region of the retina that is responsible for our central vision, and it controls our ability to read, drive a car, recognize faces or colors, and see objects in fine detail. Macular degeneration is characterized by a deterioration of this central portion of the retina. At present, macular degeneration is considered an incurable eye disease, but there are treatments that can slow down and in some cases significantly delay the progression of the disease to blindness.
AMD is often detected in an eye exam, before the symptoms become noticeable to the patient. In early AMD, tiny drusen or waste deposits can be seen on the surface of the retina. The macula itself sometimes shows a change in its color (pigment). In many people, the disease does not progress beyond this condition. If the disease has progressed further than this initial stage, symptoms can include blurred or fuzzy vision; the illusion that straight lines, such as the edge of a door or sentences on a page, are wavy; the illusion that some objects are smaller than they really are; and the appearance of a gray, dark or empty area in the center of the visual field. Sometimes color vision is noticeably paler than usual.
There are two general categories of AMD, a “dry” kind and a “wet” kind. Dry AMD is more common and is often, though not always, seen as a precursor to the wet kind. Dry AMD is characterized by a chronic and often slowly progressive deterioration of the macula, whereas the wet kind often can worsen quickly and involves the growth of new and unstable blood vessels in the macula that leak blood and/or fluid underneath or within the retina. The only treatment that research has shown to help slow the progression of dry AMD is the AREDS2 collection of vitamins/supplements, which can be bought as over-the-counter vitamins either individually or as a complete supplement under names such as Preservision, Ocuvite, or Icaps to name a few. The sudden leaking of fluid or blood in wet AMD can be treated with an injection into the eye of medications such as Avastin, Eylea, or Lucentis. The beneficial effects of the injected medication often only lasts a limited amount of time, from a few weeks to many months, and it is not uncommon for patients to require injections monthly or every few months for an extended period of time.
AREDS2 supplements, injections and appropriate follow-up care can reduce the risk of blindness. However, treatment often cannot restore vision that has already been lost to dry AMD. While treatments can often help recover some vision that has been affected in wet AMD, the longer the blood/fluid is present and undiscovered or untreated, the greater the chance of permanent vision loss. For these reasons, regular eye exams in older patients and those with known macular degeneration are important in preventing vision loss.
Glaucoma

Glaucoma is a group of diseases that damage the eye’s optic nerve and can result in vision loss and blindness. The vision loss most frequently involves the peripheral vision first and moves inward toward the central vision, but central vision can be affected even early on in some patients. Elevated eye pressure is a major risk factor for optic nerve damage and most types of glaucoma involve a pressure in the eye that is above normal. In some patients the eye pressure may be within a normal range, but is still higher than what can be withstood by the optic nerve, and damage can still ensue. Glaucoma can develop in one or both eyes.
There are several different kinds of glaucoma, with the most common being open-angle glaucoma, and others including but not limited to closed or narrow angle glaucoma and glaucoma secondary to other causes such as trauma, infection, inflammation in the eye, or congenital defects. During a comprehensive eye exam changes in your optic nerve, eye pressure, or visual field can be detected early in the disease process, and with early detection and treatment you can often protect your eyes against serious vision loss. Treatment for glaucoma is directed at lowering the eye pressure to a level at which damage no longer continues. Treatment most often involves prescription eye drops to lower the eye pressure, but can also involve pills, laser procedures, and/or surgery. While these treatments may save remaining vision, they do not improve sight already lost from glaucoma. The course of the disease is variable from patient to patient, with some patients requiring only minimal drops to keep their optic nerve from further damage, whereas other patients progress to needing additional drops, pills, laser, and/or surgery.
The most common kind of glaucoma, open-angle glaucoma, has no symptoms early on, causes no pain, and central vision stays normal. Without treatment, people with open-angle glaucoma will slowly lose their peripheral (side) vision. Eventually their vision loss will progress to the point that they will seem to be looking through a tunnel. Over time, straight-ahead (central) vision may decrease until no vision remains. As vision that is lost from glaucoma cannot be regained, early detection through regular eye exams is an important way to prevent vision loss.
Ocular Trauma

There are a myriad of eye injuries that can cause vision loss and they are among the most common preventable causes of blindness if they aren’t treated. That is why we strive to make our clinic available for you and your family should an event occur, and our staff members are highly trained in providing emergency eye care for our patients. We have same-day appointments and Saturday appointments available for these emergent or urgent needs, as well as an after-hours answering service.
Sand, dirt, or other foreign bodies can get in the eyes and cause irritation to the surface of the eye. Flushing the eye at home with eyewash or artificial tears is OK to try, as long as you don’t get overly aggressive with the flushing and cause more irritation or damage. Sometimes a particle may scratch the eye and cause an abrasion. Any break in the outer tissue of the eye, such as an abrasion, can lead to an infection, in which case the doctor will often provide a prescription for antibiotic eye drops or ointment and arrange for close follow-up.
Many chemicals, even those found around the house, can damage an eye. If you or your family member gets a chemical in the eye, flush the eye immediately with water, eye wash, saline, or artificial tears for 20-30 minutes and call for emergency medical help. Be prepared to give the exact name of the chemical if you have it. Do not delay flushing, start the flushing first and then call our office for further instruction.
Black eyes and blunt injuries are often times a minor injury. However, sometimes blunt injuries can cause fractures of the thin bones around the eye, or cause bleeding inside of or behind the eye. A visit to our office to rule out serious injury is never a bad idea, but you should definitely be examined if you are having blurry or decreased vision, double vision, pain with looking around, drainage from the eye, increased redness of the eye or around the eye, or if you aren’t sure what caused the black eye.
A foreign body or object that hits the eye can become embedded in the tissue of the eye or even penetrate the wall of the eye. An embedded foreign body or globe penetration requires an immediate call for medical help. Keep yourself or your family member as calm and comfortable as possible until help arrives or until you get to a medical facility. Do not attempt to remove the object yourself. If you are able to, give us an advance phone call so that we know you are coming and can be ready for arrival to the medical facility. A small foreign body that is embedded in the eye, but which has not penetrated the eye, can often be removed in the clinic. Larger foreign bodies and anything that has penetrated the wall of the eye will often require a trip to the operating room to repair.
Oculoplastics

Oculoplastics deals with disease and surgery of the structures around the eye. This may include the eyelids, the eyebrows, the tear system and the tissues behind the eye, known as the orbit. These structures are critical for vision. Injuries, congenital defects, aging changes and tumors affecting the eyelids as well as the tissues and bones surrounding the eyes can cause pain, eye damage, vision loss and disfigurement. Oculoplastic surgeons can correct eyelid-position abnormalities, remove growths and rebuild critical structures surrounding the eye.
Allergies

Airborne allergens including pollutants, pollens, animal dander and mold constantly bombard the eyes and can cause ocular allergies at any time. There are several new safe and effective anti-allergy drops that can be prescribed. An eye doctor can also ensure your symptoms are not being caused by a more serious problem.
Conjunctivitis

Pink eye, the most common name for conjunctivitis, is an inflammation or infection of the conjunctiva, the outer, normally clear covering of the sclera, the white part of the eye. The eye appears pink in conjunctivitis because the blood vessels are dilated. Conjunctivitis is often accompanied by a discharge, but vision is usually normal, and discomfort is mild.
Conjunctivitis is most commonly caused by either a bacterial or a viral infection, but can also be caused by allergies, irritation to the surface of the eye, dryness of the eye surface, eyelids that do not close completely, and a variety of other causes. Viral conjunctivitis, which is one of the most common types, can last several weeks, and may be associated with an upper respiratory infection (or cold) at the same time. There is no treatment for the most common kinds of viral conjunctivitis. Unlike viral conjunctivitis, bacterial conjunctivitis can be treated with a variety of antibiotic eye drops or ointments, which usually cure the infection in a few days. It can often be difficult to tell with certainty which kind of conjunctivitis you have on exam.
With either bacterial or viral conjunctivitis, it is important to take measures to prevent spreading the infection to others. Helpful tips include frequent hand washing, trying not to touch your eyes, and avoiding the sharing of towels, pillowcases, or face clothes. Make-up items that touch the eyelashes or eyelids, such as mascara wands, should be thrown away if they were used while the eye was infected, as they may re-contaminate the eye after you have healed.
Dry Eye

Dry eye syndrome is a condition in which there is an insufficient amount of or a poor quality to the tears needed to lubricate and nourish the eye. Tears are necessary for maintaining the health of the front surface of the eye and for providing clear vision. With each blink of the eyelids, tears are spread across the front surface of the eye, known as the cornea and conjunctiva. Tears provide lubrication, reduce the risk of eye infection, wash away foreign matter and irritants from the eye, and keep the surface of the eyes smooth and clear. Excess tears in the eyes flow into small drainage ducts in the inner corners of the eyelids, which drain in the back of the nose. People with dry eye syndrome may experience symptoms of irritation, grittiness, scratchy or burning eyes, a feeling of something in their eyes, excess watering, and blurred vision. Advanced dry eye syndrome may damage the front surface of the eye and impair vision.
Dry eye syndrome can be the result of either an inadequate amount of tears or a poor quality of tears, or a combination of the two. Your eye doctor can evaluate your eyes and get an idea of which of these problems you have. Dry eye syndrome is very common and often a chronic problem, particularly in older adults. The source of the dryness is usually multi-factorial and can involve weather and humidity changes, hormonal changes, medications, eyelid malposition or abnormalities, and increased use of forced air heating, just to name a few. Occasionally the dryness can be related to a more serious systemic condition, usually an auto-immune disease, such as Sjogren’s syndrome, Lupus or others. Another name for dry eye syndrome that is predominantly a lack of tear production is keratoconjunctivitis sicca (KCS).
There are many treatments for dry eyes including over the counter artificial tears and ointments, prescription medications, punctal plugs to block the drainage of tears away from the eye surface, or even surgery. Each of these methods aims to restore or maintain the normal amount of tears in the eye, to minimize dryness and related discomfort, and to maintain eye health.
Excessive Tearing

Watery eyes (epiphora) can be due to many factors and conditions.
In infants, persistent watery eyes, often with some matter, are commonly the result of a blocked tear drainage system (also called nasolacrimal duct obstruction). To further explain, the tear drainage system (called the nasolacrimal system) carries away tears, similar to how a storm drain carries away rainwater. Tears normally drain away from your eyes through tiny openings (puncta) in the inner part of the eyelids, run through a small sac called the nasolacrimal sac, and then progress through a small canal into the nose. In infants, the most common reason for excessive tearing is the persistence of a thin membrane that blocks the drainage pathway down where the tears enter into the nose, causing the drainage system to not be fully open and functioning. Your eye doctor can teach you how to massage the area to encourage an opening of the blockage. The crusting and buildup on the eyelids is not generally threatening to the child’s eye, vision, or health. If this blockage persists beyond the first year of life, it is reasonable to take the child to the operating room for evaluation under anesthesia and to attempt to open the blockage using thin probes. Occasionally the child will have small or nonexistent puncta (the opening in the eyelid where the tears drain), which can also be addressed at the time of the procedure. It is important to note that if the child develops redness, swelling, or a nodule between the lower eyelid and the nose, or seems to be tender in that area, you should call your eye doctor and seek medical care, as this could be a serious infection in the tear drainage system. There are many reasons why toddler or child can have excessive tearing, including eye irritation, allergies, foreign bodies, or abrasions. An exam from an eye doctor is recommended should your child begin to have excessive tearing.
In adults, persistent watery eyes are often a result of dryness (see Dry Eye section). Allergies or viral infections (conjunctivitis), the common cold, eye injury or foreign body in the eye, as well as any kind of inflammation, may also cause watery eyes. Excess tearing can also be related to the changes the in the eyelid tissue or position, related to aging or other causes, leading to the lower eyelids sagging away from the eyeball and allowing tears to accumulate and flow out onto the cheek instead of down the tear drainage ducts. Minor symptoms can be treated with artificial tears, tear gels, or ointments, whereas moderate to severe cases often require surgery to correct the position of the eyelids.
Excess tearing in adults can also be related to a blockage of the tear drainage system, which can be from several causes including infection, tissue changes, accumulation of debris or “stones”, and in rare cases tumors or radiation. If a blockage is suspected, the tear drainage system (nasolacrimal system) can be flushed with saline in the clinic to help determine if the system is open or not. If a blockage is present, often surgery is the recommended method to restore a normal functioning tear drainage system.
Floaters
Floaters are a common visual phenomenon, but can also signal an immediate need to see an eye care professional. Floaters are caused by tiny particles that are floating in the gel inside the eye. They are often more noticeable when looking at a white background or screen, when focusing on the floaters, or when outside looking at the bright sky. While small and often barely-perceptible floaters that have been present for years are usually not a sign of a disease or problem, the onset of one or more new, larger, darker, or more prominent floaters, or a sudden onrush or shower of small floaters can signal a need to call your eye doctor and be examined immediately.
As part of the normal aging process of the eye, the gel inside the eye (called the vitreous) will go through a process of detaching from the retina. This process, called a posterior vitreous detachment, is often associated with one or more new, prominent floaters or a shower of new tiny floaters. You may also see flashes of light in that eye, especially when you are in the dark or with turning your head or eyes. These symptoms require a call to your eye doctor and immediate evaluation. While it is a normal aging process for the vitreous gel to detach from the retina, in some patients the detaching vitreous will cause a tear in the retina, which can lead to a retinal detachment and vision loss. If a retinal tear is found on exam, a laser can be used in the clinic to help prevent the development of a retinal detachment. See the Retinal Tears & Detachments section for more information.
Occasionally increased floaters and/or flashes of light can occur with inflammatory conditions of the eye or even infections in the eye. As stated above, an immediate, thorough eye exam is recommended.
Retinal Tear & Detachment

The retina is a light-sensitive layer of tissue that lines the inside of the eye and sends visual messages through the optic nerve to the brain. When the retina detaches, it is lifted or pulled from its normal position. If not promptly treated, retinal detachment can cause permanent vision loss. A retinal detachment is a medical emergency and often requires surgery to correct.
In some cases a retinal tear or break forms first and subsequently leads to a retinal detachment. Symptoms that can indicate a retinal tear or detachment include a sudden or gradual increase in either the number of floaters, which are little “cobwebs” or specks that float about in your field of vision, and/or flashes of light in the eye. Another symptom, which is of particular concern for a possible retinal detachment, is the appearance of a dark or gray curtain or shade over any part of the field of vision. Anyone experiencing any of these symptoms should see an eye care professional immediately.
Small holes and tears are treated with laser surgery, usually performed in the doctor’s office. During laser surgery tiny burns are made around the hole or tear to “weld” the surrounding retina into place, preventing the progression of the tear to a detachment. Retinal detachments often require procedural or surgical intervention to correct.

